Dr Moon Moon Das writes how because of the widespread use of antibiotics, the target bacteria have adapted and changed with time, making the drugs less effective.
Antibiotic resistance accounts for about 700,000 deaths per year. Tedros Adhanom Ghebreyesus, the WHO director-general, has said that COVID-19 is not the last pandemic, and there are more to come. He also added that COVID has highlighted the intimate links between the health of humans, animals, and plants.
The current pandemic must have accelerated the antibiotic resistance due to its use in the patients showing COVID-19 symptoms to provide immunity against secondary bacterial infection. Professors David Graham (Newcastle University) and Peter Collignon (Australian National University) warn “the next pandemic might be worse”. They added that there is a continuous increase in antibiotic resistance, and, globalisation, hospitals, agriculture sector, industrial wastes, etc., catalyse the incidence of antibiotic resistance.
Let us understand “antibiotic resistance” first. What do we take to treat fever or a strep throat or an ear infection? The answer is antibiotics. An antibiotic is a drug that stops the growth of the infection-causing bacteria or kills it. For example, say, you went for nose or ear piercing, and after sometime, you develop an infection; a physician prescribes you a topical ointment to get rid of the infection. That topical ointment contains antibiotics that will kill the infection-causing bacteria. Alexander Fleming discovered penicillin in 1928; and later, Howard Florey, Ernst Chain, and Norman Heatley worked on it to make it available as a drug for use, and it won them the Nobel Prize in 1945. In the Nobel Prize acceptance speech, Fleming warned about the development of resistance to penicillin if overused, and he was right about this – just after two decades of its discovery, the penicillin-resistant Staphylococcus (bacteria that causes a number of diseases such as infection in skin, eyes, gastroenteritis, etc.) was detected.
Looking at the timeline of antibiotics developed so far, we see no new antibiotics in the last decade, and this crisis is of serious concern as the pathogens have turned resistant to almost all the available antibiotics. According to the Centers for Disease Control and Prevention (CDC) 2019 report, antibiotic resistance causes 25,000 deaths per year in the European Union and the US, 38,000 deaths per year in Thailand, and in India, 58,000 infants died in one year due to resistant bacteria.
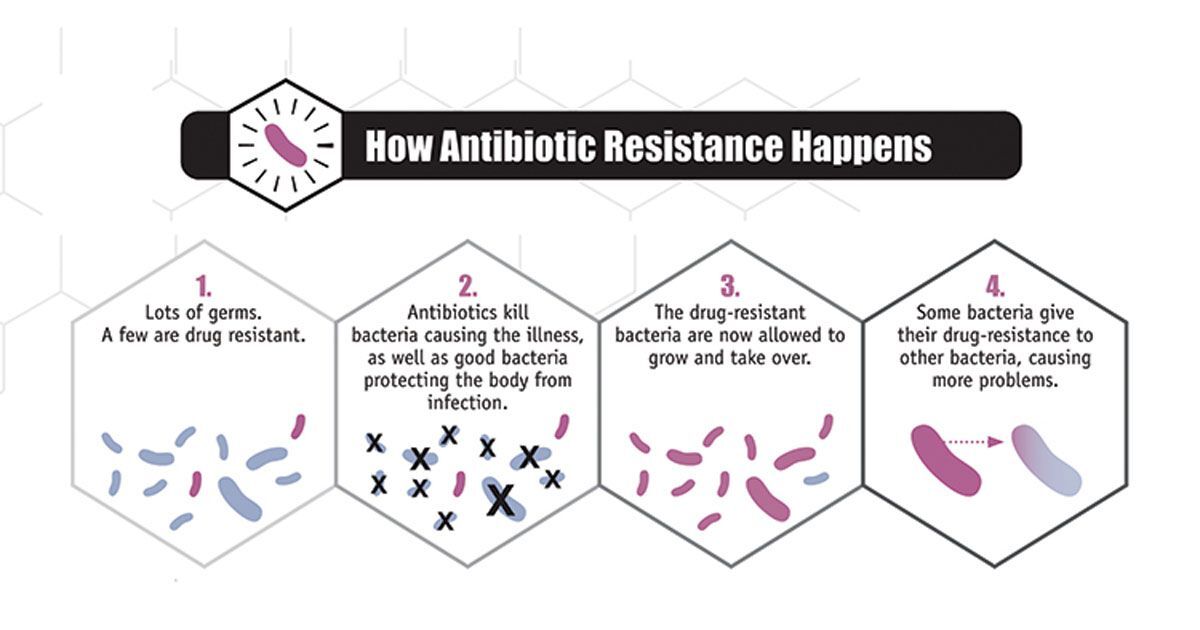
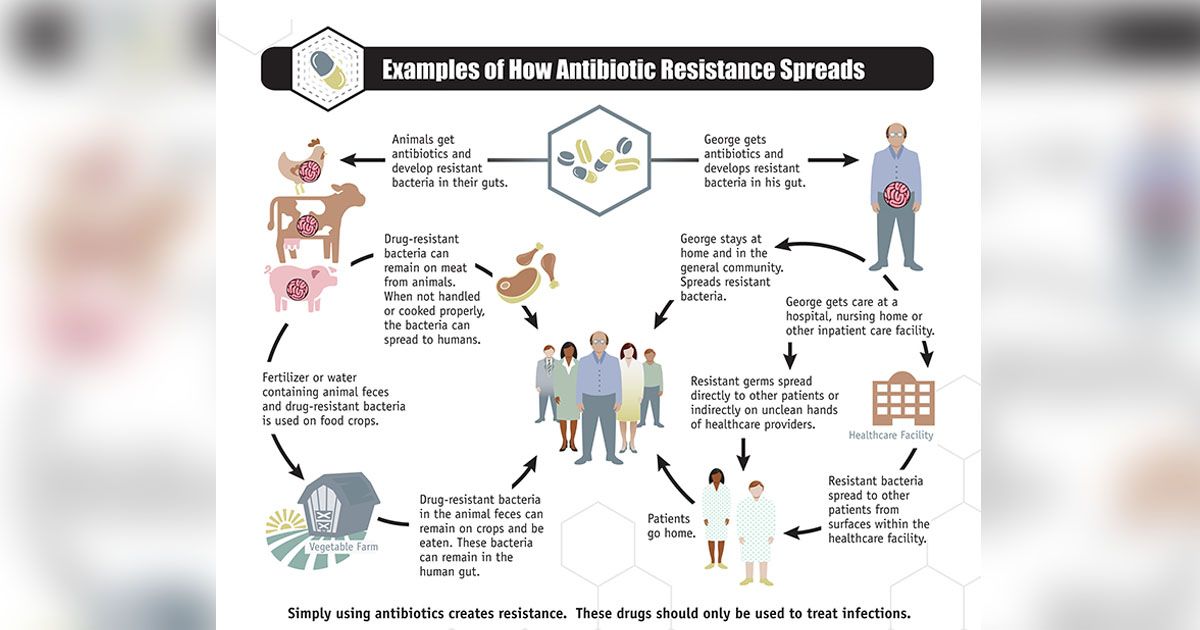
Antibiotics are prescribed during different medical procedures, be it to treat a mild fever, cancer treatment, open-heart surgery, or organ transplantation. So, to imagine a world without an antibiotic to fight the germs is scary. Now, the question is – how do the bacteria become resistant? The simple answer for this is – natural selection or the result of evolution. When an antibiotic is given to a bacterial population, some of the mutated bacteria survive, and later on, it multiplies or transfers their resistance to other bacteria, giving rise to a fully resistant population. The resistant bacteria find different ways to survive the antibiotic pressure such as throwing the antibiotic outside their cell, destroying the antibiotic, or restricting entry into the cell. The antibiotic resistance spreads rapidly across hospitals, communities, foods, and homes. It is regarded as a “One Health” problem where people’s health is connected to animals, water, soil, and air. In farms, antibiotics are extensively used in animal feed to promote animal growth. Due to excessive use of these antibiotics, they become a reservoir of antibiotic/drug-resistant bacteria, and this transfers to humans during cleaning the animal faeces, animal slaughtering, and consumption of the contaminated meat. Eating undercooked or raw meat can cause antibiotic-resistant food poisoning. It is not only with meat, but even milk, fish, vegetables, and fruits may be contaminated by antibiotic resistant germs. In a report from the Department of Biotechnology (DBT) on antibiotic resistance released in 2017, it was stated that tilapia, shrimps, clams, and shellfish from urban lakes/rivers and retail markets were contaminated with drug-resistant bacteria. According to this report, India ranks fifth in consumption of antibiotics in meats, and with dietary changes and increasing demand for meat, the use of antibiotics may rise, making India the fourth largest consumer of antibiotics by 2030; China tops in consumption of antibiotics in meat.
Though antibiotic resistance is a natural process, we can still prevent or slow down this process. WHO has taken several initiatives to address the global concern of antibiotic resistance and also declared November 18 to 24 as “World Antimicrobial Awareness Week”. CDC reports suggest that approximately 30 per cent of the prescribed antibiotics are unnecessary. Viral infection such as runny nose, common cold, flu, sore throat, etc., cannot be treated by antibiotics as they are caused by a virus and not bacteria. Antibiotics should only be used to treat diseases caused by bacteria, for example, strep throat, whooping cough, urinary tract infection, septicemia, etc. So, if we can cut down the needless usage of antibiotics, we can reduce the risk of drug resistance. To prevent antibiotic resistant transmission from foods to humans, five simple tips can be followed: cook, clean, chill/refrigerate, separate raw food from cooked food, and use clean water. Washing hands properly, cleaning raw meat/fish/vegetables/fruits, and cleaning the cooking area should be practised. We should all be aware of the antibiotic resistance issue, which, if ignored, can worsen the current situation. We are already in the post-antibiotic era, with no novel antibiotics, and some bacteria are already resistant towards the last resort of antibiotics. We should use antibiotics only when it is really necessary so that we can save ourselves and the future generation.

